
Claudia, a nurse at the Pedro Ernesto University Hospital post-COVID-19 care unit in Rio de Janeiro, takes care of a patient
RIO DE JANEIRO: Her voice temporarily silenced by a nearly three-month battle with COVID-19, Elenice da Silva “talks” by mouthing her words in a Brazilian care unit created to help hard-hit patients recover their health and their lives.
“I’m doing great,” the 63-year-old tells her physical therapists with her lips in the post-coronavirus treatment center at the Pedro Ernesto University Hospital (HUPE) in Rio de Janeiro.
The unit was created to help patients like her, who have overcome severe cases of COVID-19 but now need further specialized care to deal with the after-effects.
That is the case for a surging number of people in Brazil, the country hit second-hardest by the pandemic, after the United States, with nearly 2.2 million infections.

Staff check on Elenice da Silva’s tracheotomy in the post-COVID-19 care unit
More than 80,000 people have died of the virus in the South American country, according to official figures.
Nearly 1.5 million have recovered. But there is another troubling problem behind that more-hopeful statistic: often, those who survive severe cases of the virus face a long, hard road to regain their health.
“They are socially vulnerable (patients) who have recovered from the initial stage of their illness … but still need multidisciplinary assistance,” said Marcia Ladeira, one of the specialists coordinating the unit.
After long stays in intensive care, patients are often left suffering from atrophied muscles or problems affecting their lungs, hearts or kidneys.
Many have other underlying conditions and need longer-term care including an array of therapies: physical, nutritional, psychological, and hearing and speech, Ladeira told AFP.
“Our care team creates an environment where these patients can fully recover and leave here walking and eating on their own, without feeding tubes, with their bed sores healed. Ready to reintegrate into society,” she said.
The hospital opened the unit during the worst of the pandemic in Rio, where the health system was pushed close to the breaking point from April to June.
The unit has treated dozens of patients, though the numbers have declined now that new infections are no longer rising exponentially. Just five people were recovering there on a recent visit.
GIANT CAKE
Patients spend anywhere from one week to several months in the post-COVID unit.
Da Silva, who also has epilepsy and other underlying conditions, is strengthening her arms and legs with the help of two physical therapists, learning to stand up again in brief intervals.
“Intensive care was awful. But now I’m feeling marvelous. If not for these doctors … I would have died,” she said, this time speaking with the help of a valve placed in a hole in her trachea.
Using the device, she manages to speak for several minutes, albeit with difficulty, and has been able to talk to her children during visits.
“Her infection left her very weak … (but) she’s doing very well,” said one of her physical therapists, Cleiton Ferreira dos Santos.
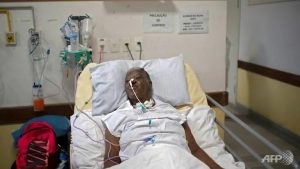
Elenice da Silva practices breathing exercises in a post-COVID-19 care unit at the Pedro Ernesto University Hospital in Rio de Janeiro
The treatment team’s next goal is to help her be able to swallow again so she can eat normally and her feeding tube can be removed.
She still has a long way to go. But she already has plans for when she leaves the hospital.
“I’m going to bake a giant cake for everyone,” she said.

